Enterprise Products
System-level transformation, now enabled by three core products
How It Works
Phare delivers better outcomes by improving throughput, reducing cost to collect and boosting yield. Here’s how:
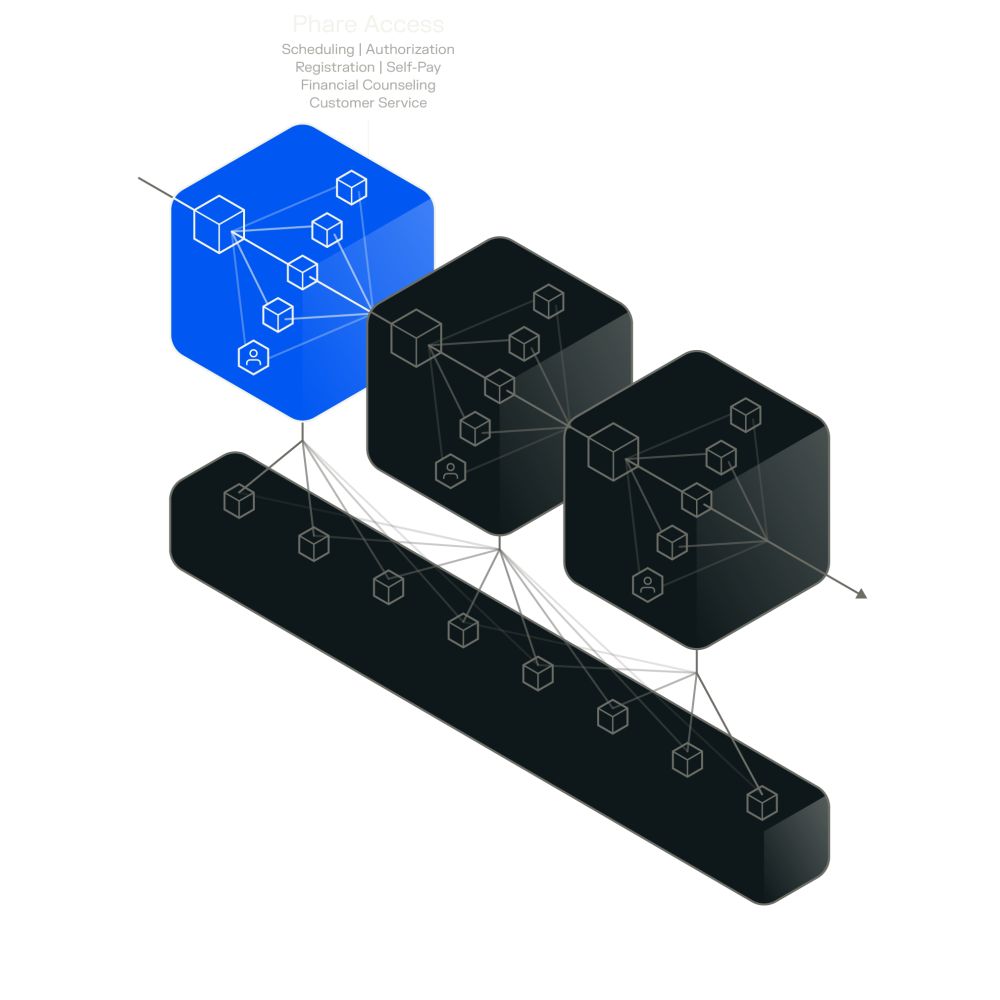
Phare Access
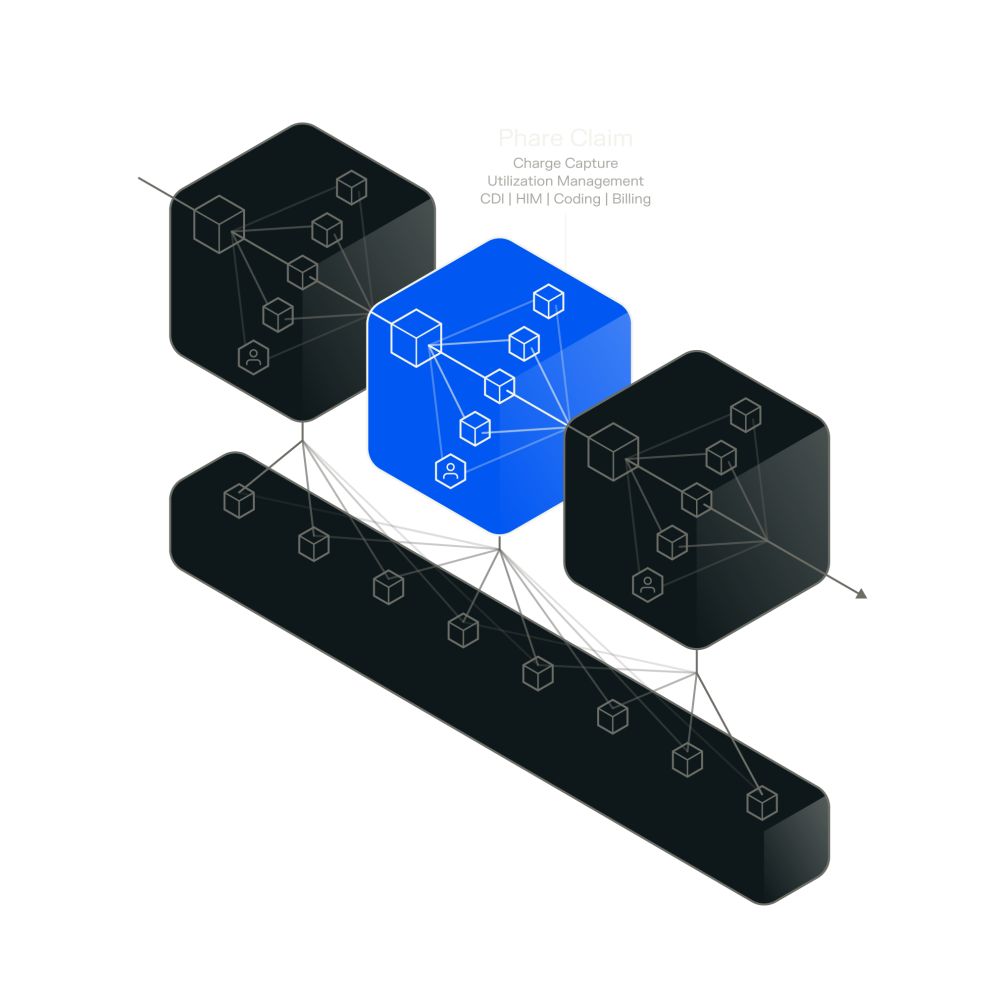
Phare Claim
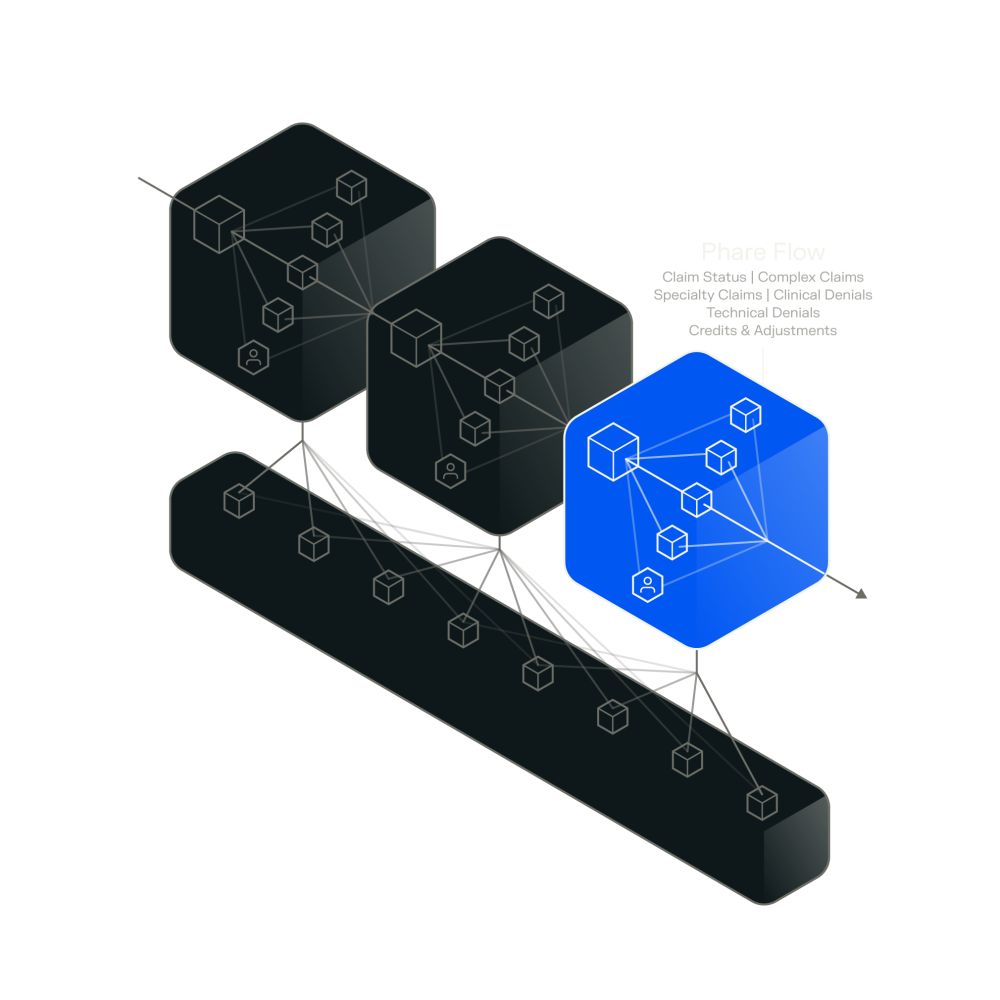
Phare Flow
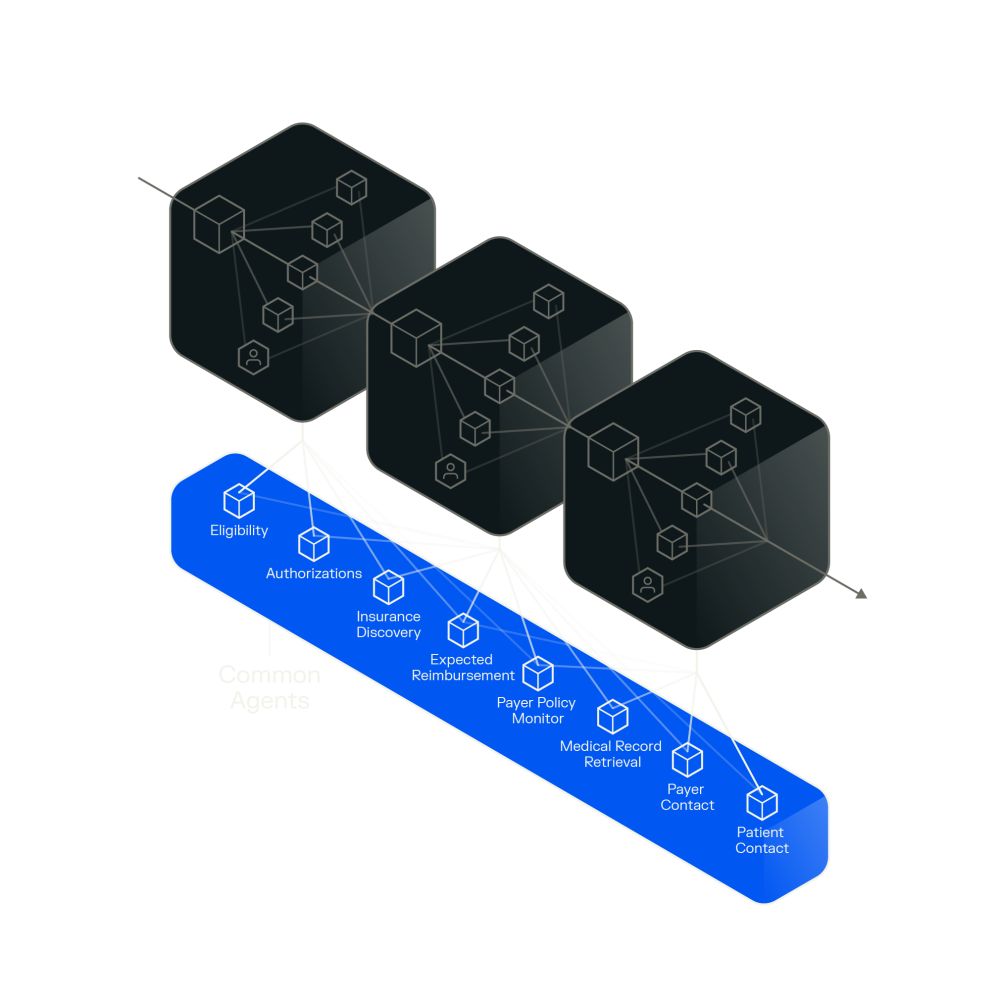
Common Agents
By pairing real-world operator experience with enterprise-grade AI and automation, we help providers reduce costs, increase revenue and streamline operations.
5-7%
net revenue improvement
50%
reduction in cost-to-collect
60%
improvement in throughput
92%
patient satisfaction












